Our Inner Healing Intelligence: What Women Lost When We Leaned In
Something is happening underneath the achievement.
What is Really Going On in Your Relationships - Why We Get in Bed with Our Unfinshed Business!!
Relationship Advice that really works!
The Gilded Cage: Achievement Pressure and the Quiet Crisis in Affluent Families
When success becomes the only language spoken at home, something essential in our children goes silent.
Finding Calm in the Chaos: Managing Anxiety Through Food and Hormone Balance
For many women, anxiety isn't just "in the head"—it’s a full-body experience.
Better Ways to Parent the “Anxious Generation”
Parenting has always been a challenging journey, but the advent of the digital age has introduced unprecedented complexities.
Neurofeedback: A Smarter Way to Train the Brain
Discover how to use narrative therapy techniques in a simple journal practice to rewrite limiting stories and promote personal growth.
The GutBrain Axis How Microbiome Diversity Influences ADHD and Anxiety
Gut/Brain Axis in understanding you mental and physical health
The Hoffman Process: A Transformative Journey of Self Discovery
Journey through the family of origin to find lasting change.
The New IQ: Why Emotional and Flexible Intelligence is the Human Edge in an AI World
AI is changing what and how kids need to learn
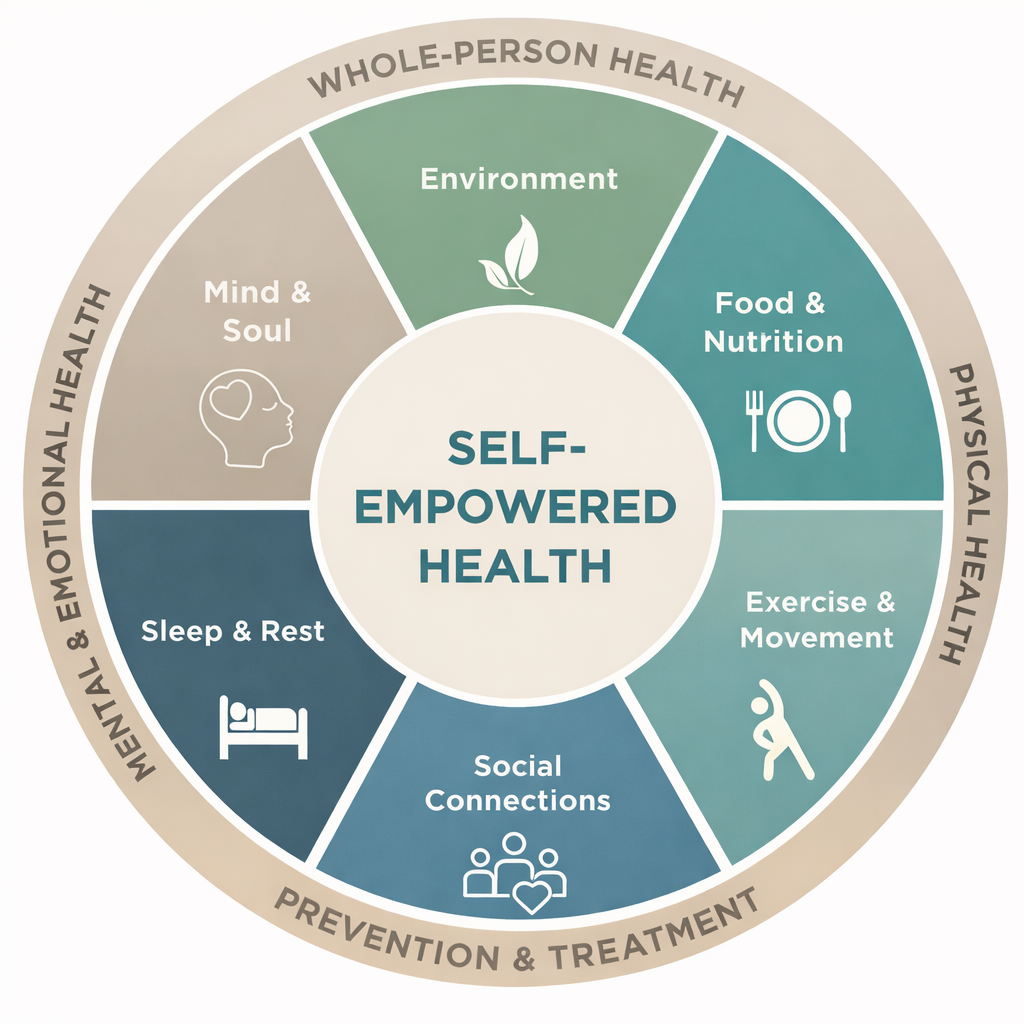
The Foundations of Self-Empowered Health: A Whole-Person Approach to Mental Well-Being
Whole person approach to mental strength
The Importance of Counseling in Achieving Long-Term Goals
Touching the source and finding the long term goals